Eye diseases and conditions
Diabetic Retinopathy
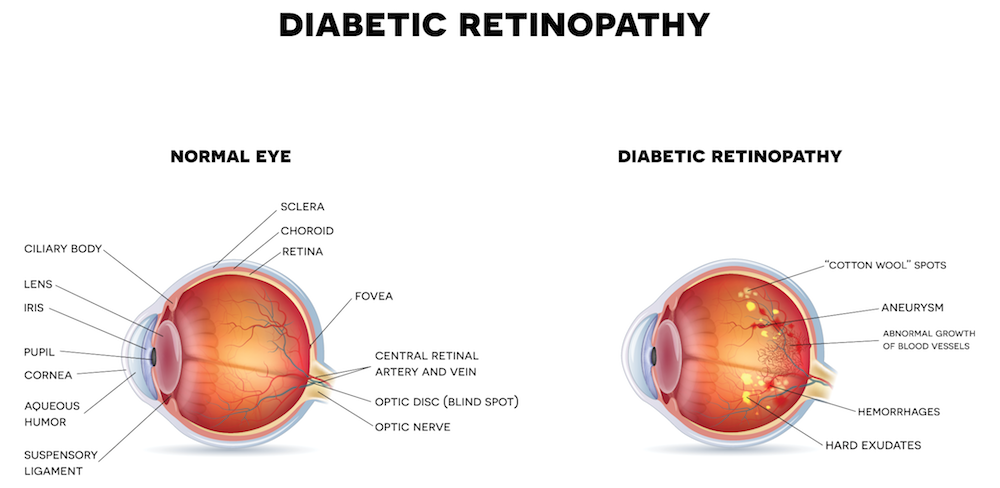
Diabetes causes your body to have difficulty managing sugar levels within the bloodstream. Over time, high levels of blood sugar can lead to damage in the tiny vessels in your retina. This is called diabetic retinopathy. There are various stages of diabetic retinopathy. In the earliest stage, there may only be mild leakage of blood or fluid from the retinal vessels. If this swelling occurs in the central portion of the retina, it causes macular edema, the most common cause of vision loss in diabetics. The more advanced stages of diabetic retinopathy cause ischemia, which is when the small blood vessels close off and block blood flow to the retina. The body has a natural response to this, which is to form new blood vessels in an attempt to increase blood flow. These new vessels tend to leak, which in turn causes even more problems. These problems include: vitreous hemorrhage (bleeding into the space within the eye); tractional retinal detachment (scar tissue that forms from diabetic retinopathy pulls on the retina causing a detachment); and neovascular glaucoma (a blockage of fluid outflow from the eye, causing a painful loss of vision due to high eye pressure).
Regular eye exams are important as a diabetic. Diabetic retinopathy can be diagnosed and treated before you experience vision loss. Treatments include laser, injections into the eye, and a procedure called a vitrectomy, which removes the vitreous gel of the eye and the leaky blood vessels associated with it. The goal of these treatments is not to restore vision that’s been lost already, but to prevent further deterioration. The most important thing to know about vision loss from diabetic retinopathy is that it is preventable. You should plan to have an eye exam at least yearly, and possibly more often, if you have risk factors for vision loss.

